A pressure ulcer (decubitus ulcer) is a localized injury to the skin and/or underlying tissue, usually over a bony prominence. This type of ulcer is the result of pressure, or pressure in combination with shear (2). The pressure prevents the blood from circulating properly, and causes cell death, tissue necrosis and the development of ulcers. Wheelchair users or people confined to a bed (for example, after surgery or an injury) are especially at risk.
Major cause of morbidity
Pressure ulcers are a major cause of morbidity and mortality, especially for people with impaired sensation, prolonged immobility, or advanced age. The most common places for pressure ulcers are over a bony prominence, such as elbows, heels, hips, ankles, shoulders, the back, and the back of the head.
Classification
Pressure ulcers are classified according to the degree of tissue damage observed. In 2009 the EPUAP-NPUAP advisory panel agreed upon four levels of injury (3):
Category/Stage I: Non-blanchable redness of intact skin
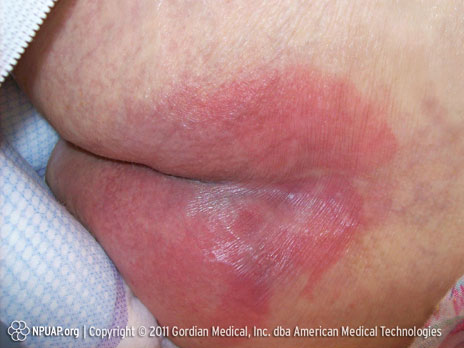
Buttocks, Stage I, NPUAP copyright & used with permission.
Intact skin with non-blanchable erythema of a localized area, usually over a bony prominence. Discoloration of the skin, warmth, edema, hardness or pain may also be present. Darkly pigmented skin may not have visible blanching.
Category/Stage II: Partial thickness skin loss or blister
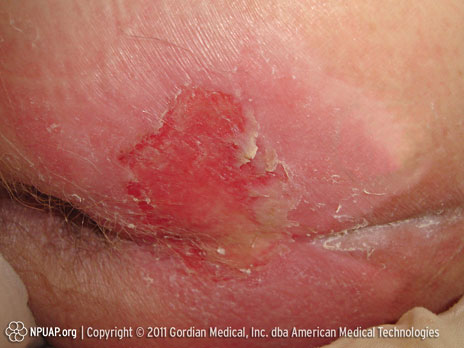
Buttocks, Stage II, NPUAP copyright & used with permission.
Partial thickness loss of dermis presenting as a shallow open ulcer with a red-pink wound bed, without slough. May also present as an intact or open/ruptured serum-filled or serosanginous-filled blister.
Category/Stage III: Full thickness skin loss (fat visible)
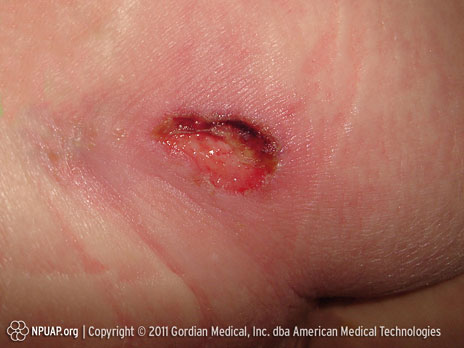
Ischium, Stage III, NPUAP copyright & used with permission.
Full thickness tissue loss. Subcutaneous fat may be visible, but no bone, tendon or muscle is exposed. Some slough may be present. May include undermining and tunneling.
Category/Stage IV: Full thickness tissue loss (muscle/bone visible)
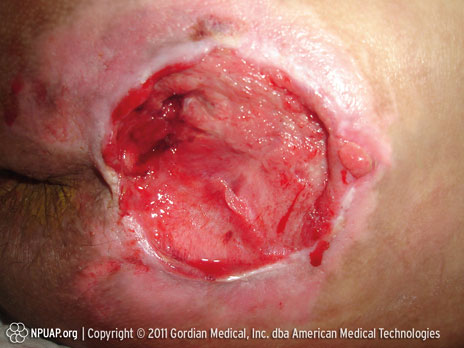
Sacral Coccyx, Stage IV, NPUAP copyright & used with permission.
Full thickness tissue loss with exposed bone, tendon or muscle. Slough or eschar may be present. Often include undermining and tunneling.
Category/Stage: Unstageable
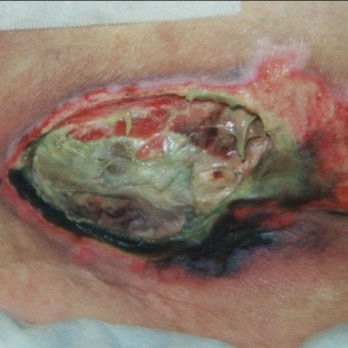
Full thickness skin or tissue loss in which actual depth of the ulcer is completely obscured by slough (yellow, tan, gray, green or brown) and/or eschar (tan, brown or black) in the wound bed.
Treatment needs (2,3)
- Pressure must be relieved or removed by appropriate measures.
- Wound care must be optimised by:
- Debridement of necrotic tissue
- Appropriate cleansing of wound and surrounding skin
- Use of appropriate moist wound healing dressings
Suitable wound dressings for pressure ulcers are foam or alginate dressings with superior absorption and exudate management properties, such as Biatain Silicone or Biatain Adhesive foam dressing or Biatain Alginate dressing. A silver-releasing dressing such as Biatain Ag or Biatain Alginate Ag can help prevent or resolve wound infection.
Download our tips for preventing, assessing and treating pressure ulcers:
Pressure ulcers – prevention and treatment: A Coloplast quick guide (pdf)